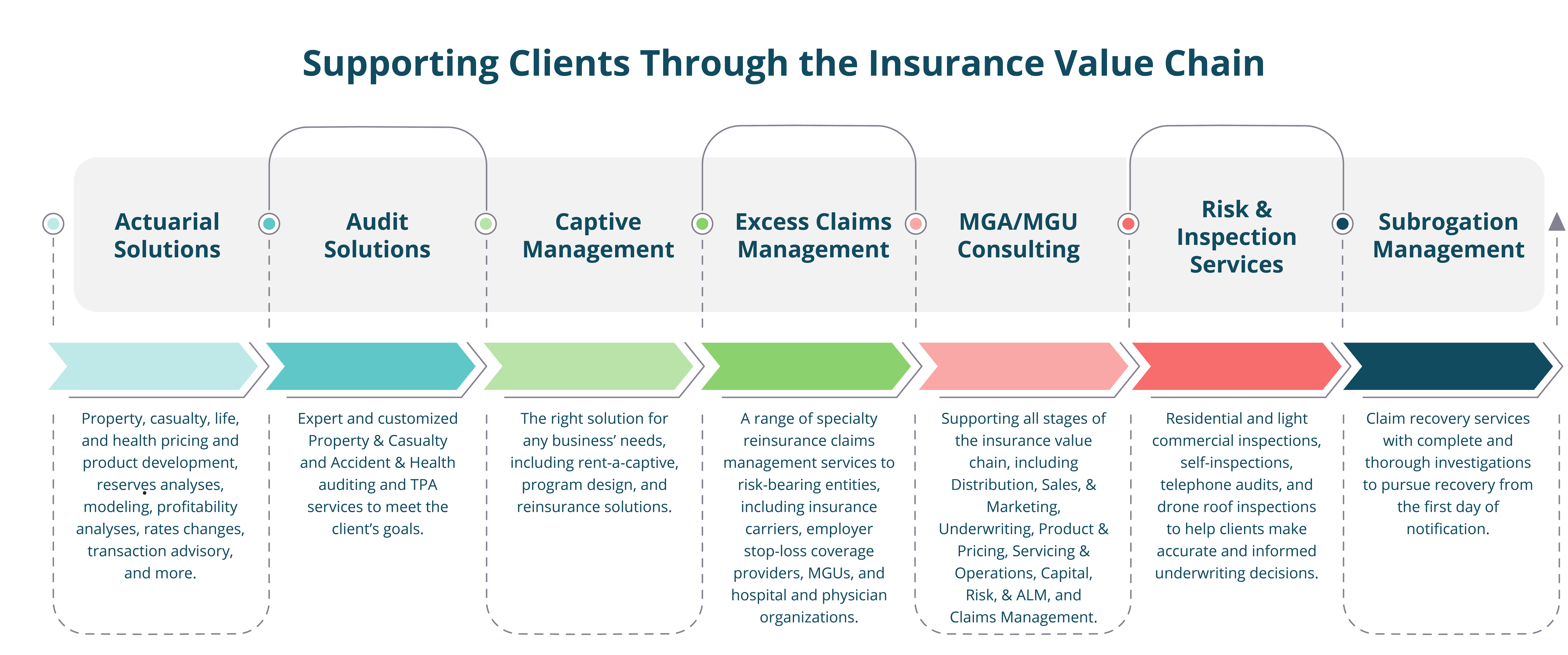
Insurance Services Solutions
Learn more about what our experts can do for you.
Audit Solutions
Our auditing team provides specialized services for the insurance and reinsurance communities. This talented team of individuals, many of whom are former insurance or reinsurance company underwriters and claims managers, have diverse expertise in personal and commercial lines, professional liability, international risks, risk management, and reinsurance. We pride ourselves on a collaborative approach with insurers, managing agents, TPAs, and brokers.
Subrogation Management
Our strategic sourcing and claims recovery experts tailor the right solutions to meet our clients’ unique needs. They have extensive coverage and liability knowledge and use a proprietary recovery tracking platform. With the latest market intelligence, we seamlessly facilitate your subrogation management and claims recovery needs.
Excess Claims Management
Through significant industry experience, advanced technical solutions, and highly skilled staff, we deliver exceptional claims reviews. We work with our clients to help manage the entire claims process as an extension of their in-house claims department.
Actuarial Solutions
We offer our clients actuarial, product development/management, regulatory compliance, and risk management consulting services to help them make informed decisions and develop strategies that best fit their business needs. Our experience gives us a unique perspective to provide clear and concise solutions that not only capture key financial measurements but can also be easily interpreted by senior management. No matter the project or goal, we work with our clients to provide custom solutions that are intuitive with the goal of optimizing operations.
Risk Services
The Davies risk services team provides full-scale, nationwide inspection services and field underwriting support for the property and casualty industry. Our professionals combine traditional inspection methods with innovative AI for more precise and near-instant analysis of industrial, commercial, and residential properties.
Captive Management
Our team delivers full service captive capabilities including feasibility studies, incorporation services, reinsurance and insurance advice, complete and ongoing management services, and exit solutions. Our expansive industry network enables us to create the right solution for our clients and to determine the necessary risks and layers of protection.
MGA/MGU Consulting
We operate as an independent incubator platform offering a “launch and host” service to entrepreneurs, private companies, and corporate entities looking to establish a Managing General Agent (MGA). We also deliver professional support services to existing fully authorized MGAs and general service support to companies active in the delegated underwriting arena.
Download Our Free Brochure